Osteoarthritis
May is Arthritis Awareness Month in the United States. Spearheaded by the Arthritis Foundation, Arthritis Awareness Month aims to make people more aware of Arthritis and the issues involved. According to the CDC (Centers for Disease Control and Prevention), 22.7% of the adult population in the US have some form of arthritis.Middle-aged and older […]
Carpal Tunnel Syndrome
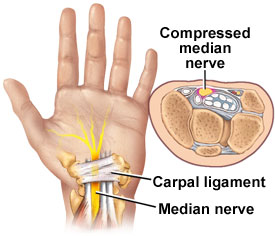
More than 2.8 million nonfatal workplace injuries were reported in 2012, according to estimates from the Survey of Occupational Injuries and Illnesses conducted by the U.S. Bureau of Labor Statistics. Hours lost for recuperation time from nonfatal injuries do nothing to help the worker or the employer. So, preventing injury and helping the worker return […]





